Dr. Sershon, United States: Setting new standards with data-driven efficiency
As patient volume grew at Harborside Surgery Center, orthopedic surgeon Dr. Robert Sershon was driven by a clear goal: to deliver high-quality outpatient joint replacement care while scaling his practice responsibly.
Over the years, Dr. Sershon had established a well-organized operating room (OR) workflow. By standardizing surgical steps and establishing a predictable rhythm across two ORs, he consistently performed 9 joint replacement procedures within a standard eight-hour OR day. His focus on clinical excellence, patient satisfaction, and team well-being had positioned his practice among the strongest examples of ASC efficiency.
However, as volume continued to increase, Dr. Sershon recognized that sustaining quality at scale would require even greater precision in how time and resources were managed.
A data-driven approach to operating room optimization
Intrigued by DEO.care’s data-driven approach to OR optimization, Dr. Sershon partnered with the team to gain objective, granular insight into his OR performance.
The DEO.care team started by capturing a detailed baseline measurement of the OR workflow and then used digital twin simulations to model how the system behaved under real clinical conditions. This comprehensive analysis revealed opportunities to further refine the process workflow.
These findings were translated into change modules and shared with Dr. Sershon and his OR team in a collaborative workshop. Following the session, the OR team implemented targeted adjustments that reduced idle time, emphasized parallel processing, and improved communication and coordination – all without extending the surgical day or compromising care standards.
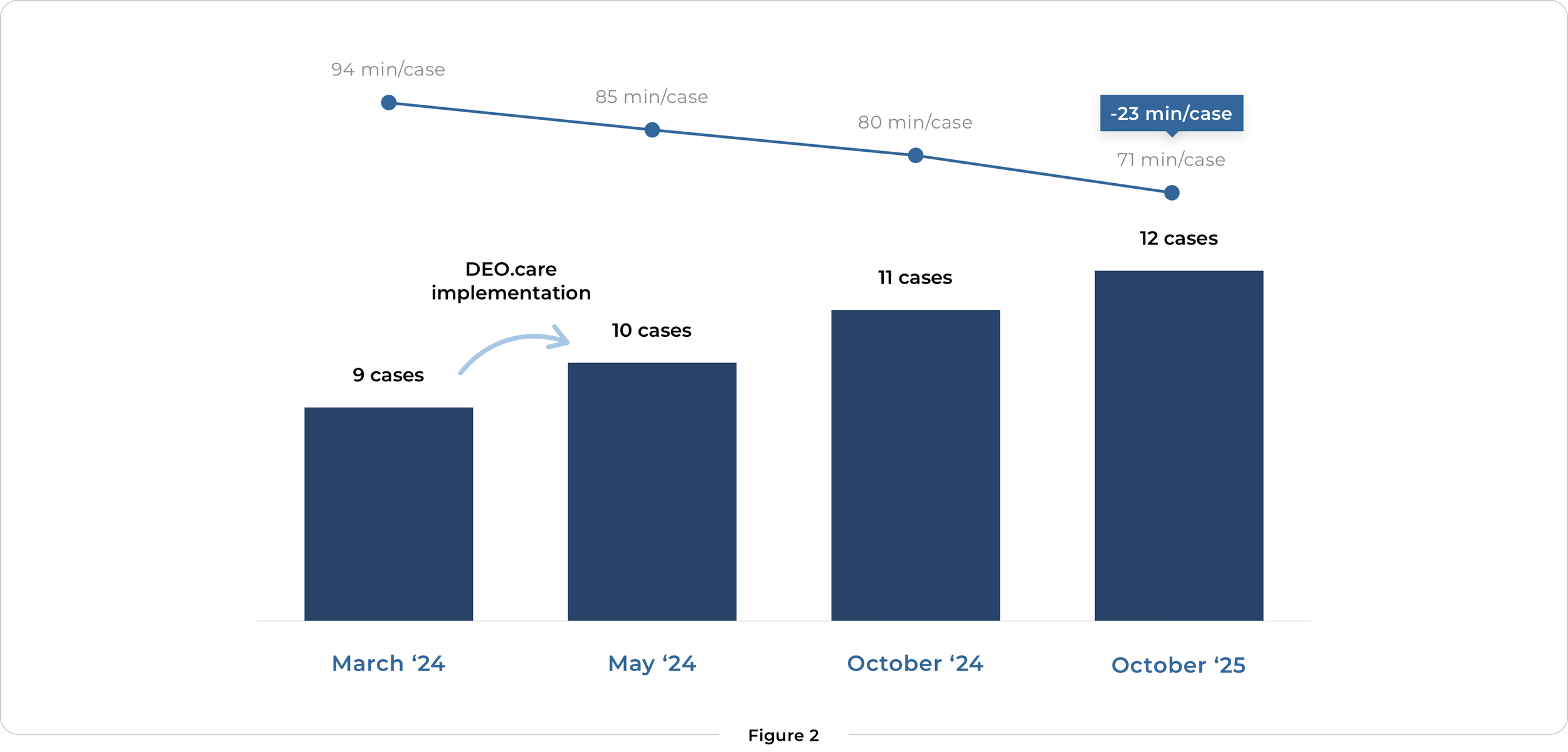
Dr. Sershon added 1 additional total joint to his 8-hour block after implementing the first cycle of changes recommended by DEO.care
The result was immediate and measurable. Within the same eight-hour block, the team added one additional joint replacement case. What had been a 9-case day became 10, achieved not by working longer but by working smarter.
From workflow improvement to sustained impact
The entire team felt the impact of the change. Sara Redden, OR Manager, noted that despite adding one more case to the day, the team did not experience an additional strain on their energy or time. In fact, the changes made the day feel smoother and more manageable while improving productivity at the same time.
Most importantly, what began as a data-driven improvement cycle quickly evolved into something more lasting. The visibility into data and insights did more than change the schedule. It changed how the team thought about flow, coordination, and excellence. Efficiency became a shared commitment, owned by surgeons, nurses, and techs alike.
Dr. Sershon’s team internalized the learnings and began proactively identifying new opportunities to improve. The OR evolved into a highly synchronized environment.
Key efficiency principles like parallel processing, clear communication, limiting idle times and refining techniques became second nature. Each member of the team understood their role: deliver exceptional care while protecting the rhythm of the surgical day.
With this mindset firmly embedded, improvements compounded. Over time, the disciplined application of these principles enabled the team to reach 12 joint replacement cases within eight hours, and today 13 cases are regularly scheduled. This level of throughput reflects both operational precision and sustained team alignment.
Over time, Dr. Sershon's team continued to refine their processes based on efficiency principles to further increase throughput in their 8-hour block
In high-performing surgical environments, efficiency is not a destination. It is a continuous journey of learning, adapting, and raising the bar, all in service of expanding access to exceptional patient care.